An aneurysm is a prominent lump filled with blood in the outer covering of any blood vessel.
Table of Contents
Where Do Aneurysms Usually Occur?
They usually occur in arteries located in the bottom portion of the brain.
The characteristic of an aneurysm is to eventually increase in size, and when it does, there is a high risk of it bursting, resulting in severe internal bleeding or hemorrhage.
Many more complications may arise, and it could prove fatal for the patient.
Aneurysms occur either due to hereditary factors or to certain diseases. In both cases, it weakens the walls of the blood vessels due to the extra strain it generates.
Aneurysms of the Posterior Inferior Cerebellar Artery are extremely rare and constitute only 0.5% of all aneurysms that are known to occur in the intracranial region of the human body.
These aneurysms are generally known to occur at the point where the Posterior Inferior Cerebellar Artery (PICA) originates from the vertebral artery.

Cerebral Aneurysms and PICA Aneurysm
PICA aneurysms in the peripheral region are even more uncommon and most of them assume a shape similar to a sac and are found only singly in number.
Even rarer is the incidence of multiple aneurysms of the Posterior Inferior Cerebellar Artery.

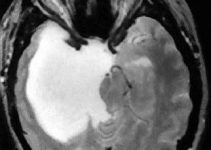
Sagittal FLAIR image showing a large extrinsic vascular mass compressing the brain stem and fourth ventricle
Aneurysms originating from more distant PICA sections are called distal aneurysms and are extremely uncommon, with a prevalence of 0.28% to 1.4% of all possible aneurysms of the cerebral region.
Multiple distal aneurysms of the PICA are exceptionally unusual, with only 11 cases having been reported to date; the first case only came to light in 1982.
Of these 11 cases, the age range was 27 years to 68 years, with an average age of 54.
There were 3 men and 8 women, with two to five aneurysms reported per artery per patient on an average — taking the total number of aneurysms to thirty.
Fifteen of these were positioned on the telovelotonsillar section. All other patients except one showed subarachnoid hemorrhage (SAH). Only one case out of these could be related to fibromuscular dysplasia (FMD).

Symptoms
An aneurysm in its initial stage is rarely known to produce any symptoms. However, just before an expanded aneurysm burst the patient is likely to show some or all of these symptoms, under two of the following conditions:
1) If an aneurysm ruptures and causes blood to flow into the region around the brain, it is called a “subarachnoid hemorrhage.” It could cause the following symptoms depending on the quantity of blood:
- an abrupt and severe headache that can go on for days
- losing consciousness
- a feeling of nausea and/or vomiting
- vision impairment
- no symptoms at all
- sudden drowsiness and/or slipping into a coma
2) If an aneurism ruptures, causing blood to flow directly into the brain, it may cause irreparable damage to the brain and this condition is known as a “hemorrhagic stroke” causing:
- debilitation or partial/complete paralysis of a limb
- difficulty in speaking or comprehending language
- difficulty in seeing
- convulsions
Treatment
To determine an appropriate surgical approach to distal multiple aneurysms of the Posterior Inferior Cerebellar Artery, the most significant aspect is to know the point of origin of the aneurysm.
At this point, either a midline suboccipital or a paramedian craniectomy can be executed, depending on where the aneurysms are situated. For all aneurysms positioned on the frontal or lateral medullary sector of the
Posterior Inferior Cerebellar Artery, a lateral mode of access should be preferred, as a superomedial retraction of the cerebellum is simple using this method. For tonsillomedullary, telovelotonsillar and cortical parts of the PICA, which are more distal forms, a midline suboccipital craniectomy is chosen since easy contact with the vermis and the 4th ventricle can be established.
Snipping the neck of an aneurysm via surgical clipping remains the best bet for all aneurysms of the peripheral regions of the PICA.
For all PICA aneurysms which arise proximally, surgical neck clipping of the aneurysm is crucial. This is because the process of getting a hold of the aneurysm could mean considerable compromise, resulting in puncturing the critical arteries in the brainstem.
Another treatment option is endovascular coiling, which was pioneered in 1991 at UCLA by Guido Guglielmi.
First, a catheter is passed into the femoral artery located in the groin region and subsequently reaching the aorta, then to the arteries in the brain, and lastly into the aneurysm.
Platinum coils are used which initiate a clotting effect in the aneurysm. If successful, this method eliminates the aneurysm.
A large amount of research has gone into discovering a suitable explanation for the occurrence of multiple aneurysms positioned in a distinct PICA, but an answer is yet to be found.
Researchers and doctors initially suspected that an infectious component of these aneurysms might be the cause of their spread.
Possible infection of the vascular wall by a septic embolus and subsequent distal migration was hypothesized as a cause of multiple aneurysms.
However, pathological tests did not support this theory. It was therefore established that infectious aneurysms are extremely unlikely.
A past study of origin for various multiple aneurysms of the PICA like FMD, polycystic kidney, polyarteritis nodosa, and other vasculitis has also been carried out.
However, the normal post-surgical angiographic reports of the aorta and arteries in the regions of the skull and kidney, the absence of any particular concerns being revealed in echocardiography, as well as normal CT scans of the abdomen excluded any of these as etiologies in most cases.
For distal PICA aneurysms, congenital reasons may have a decisive role in its pathogenesis in some of the patients.
Prognosis
The likely outcome of a ruptured aneurysm of a Posterior Inferior Cerebellar Artery depends on a multitude of factors, including the size and position of the aneurysm, and the patient’s age, medical history, and neurological health.
In some patients, the initial bleeding resulting from a ruptured PICA aneurysm leads to death. Other patients with this type of aneurysm recuperate with slight or no neurological problems.
The most noteworthy factors which are decisive in predicting an outcome are the grade of the aneurysm and a patient's age. Usually, individuals brought into Emergency with grade I and II hemorrhage, and those in a younger age bracket can anticipate a positive outcome, barring fatality or enduring disability.
Older individuals and ones with a higher grade of severity when admitted have a higher chance of a poor prognosis.
Overall, dealing with PICA aneurysms is difficult, as this is an extremely tough lesion that is prone to rupture during the course of treatment.
In some cases, patients show a good response to endovascular coiling, which requires the occlusion of the PICA. In other cases, surgical clipping shows good end results.
Commonly, almost two-thirds of individuals with this condition will experience fatality or permanent disability.
References: