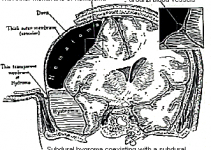
Arteriovenous malformations are masses of abnormal blood vessels that grow in the brain.
They consist of a blood vessel “nidus” (nest) through which arteries connect directly to veins, instead of through the elaborate collection of very small vessels called capillaries.
Some people are born with the nidus, but as the years go by, it tends to enlarge as the great pressure of the arterial vessels cannot be handled by the veins that drain it.
This causes a large collection of worm-like vessels to develop (malformed) into a mass capable of bleeding at some future time.
These malformations are most likely to bleed between the ages of 10 – 55; after 55, the chances of bleeding diminishes rapidly. Before 55, the likelihood of hemorrhaging is between 3 and 4% per year (with a death incidence of about 1%).
Once an AVM patient has hemorrhaged, the risk of having another one might approach 20% during the first year, and gradually lessen to about 3 – 4% over the next few years.
AVMs can occur in any area of the brain and maybe either small or large. When they hemorrhage, they usually do so with a limited amount of blood, unlike the hypertensive hemorrhages of other stroke patients.
The loss of neurologic function depends on both the location of the AVM and the amount of bleeding. Many patients have very small hemorrhages, often multiple.
They may have convulsions before even knowing about the presence of an AVM. Some patients suffer from headaches, often unrelated to the AVM, which is usually found with a CT scan or brain MRI.
In rare instances, children are born with large AVMs and are found to have heart failure because the malformation makes the heart work beyond its capacity.
These lesions are surrounded by a very discrete layer of abnormal, nonfunctioning brain tissue, thus allowing their removal with relative safety from the surrounding brain.
This factor is of the utmost importance to the brain surgeon, who can take advantage of this natural separation between normal brain tissue and the abnormal vascular malformation.
Table of Contents
TREATMENT OPTIONS

Radiation
If it is a very small AVM, and it is deep-seated in the brain, the patient is fortunate. It is possible to give focused beam radiation to the malformation and avoid surgery. Within two years the malformation will most likely disappear.
Embolization
Larger malformations may be made more surgically manageable with a technique called embolization.
With this procedure, an angiogram becomes a therapeutic tool. The interventional angiographer is capable of filling the malformation with agents that help decrease the blood supply to the malformation (coils, glues, plastic spheres, balloons, etc).
This makes surgery easier in some cases. The technique has been used as a primary treatment as well and has been successful in some cases.
Surgery
Perhaps surgery is still the best way to go if the decision has been made to do something to eliminate the AVM for good.
Surgery cures these lesions by totally removing them, thus preventing them from ever recurring again. The author's personal bias is that most AVMs are best cared for with surgical removal.
Even with patients who have large and complex arteriovenous malformations, surgery provides the cure when the malformation is completely removed.
Today, with the assistance of BrainLab's most sophisticated equipment and computerized techniques, AVM removal has been greatly facilitated.
Leave It Alone
Some lesions, because of their size, location or behavior are best left alone. In these cases, your surgeon's judgment is of the utmost importance.
In other cases, courses of treatment may be determined by the age or medical condition of the patient.
An example might be that of an AVM being found in a 70-year old woman suffering headaches after her heart surgery, having had no prior history of problems relating to the malformation.