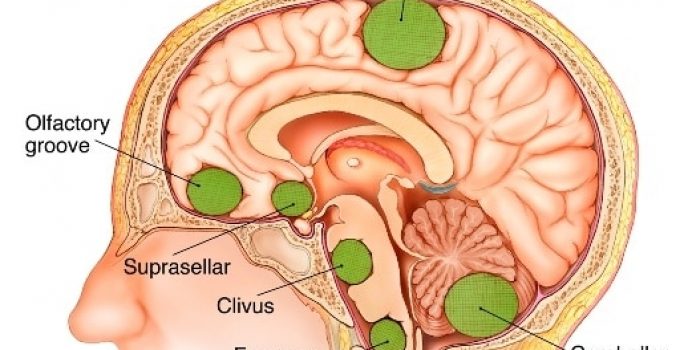
Meningiomas are tumors that begin developing in the durable membranes that protect the delicate brain. This system of thin membranes is known as the meninges and consists of three separate layers.
They include the Dura mater, the Arachnoid mater and the Pia mater. The majority of meningiomas are benign and can develop in any part of the brain or spinal cord lining.
Table of Contents
After Meningioma Brain Surgery
However, about ninety percent of all cases have been found to be either within the skull, at the skull base or just above the spinal cord.
Rarely, they can develop around the cord or the sheath that envelops the nerve that runs from the eye to the brain.
These tumors are non-cancerous and constitute the most common type of primary brain tumor.
According to the latest medical reports, every year around 4,500 individuals in the UK are diagnosed with these usually docile types of tumors.
The incidence is quite high in people of middle age and older and is more frequent in women than in men.
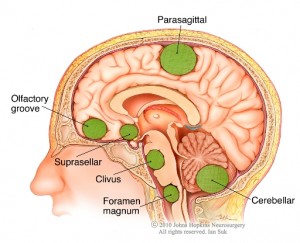
Cause
The definitive cause of the initiation, growth or recurrence of meningiomas has not yet been elucidated, but it is certainly linked to genetic and environmental factors. People with type II neurofibromatosis have been found to have this benign tumor.
Signs and Symptoms
These brain tumors are characterized by slow growth and many actually remain asymptomatic throughout one’s life. Other cases detected as benign require only periodic observation.
However, symptomatic cases can arise due to elevated pressure within the skull. This pressure occurs because of blockages in the fluid-filled ventricles in the brain, leading to an accumulation of cerebrospinal fluid.
Sometimes swelling of the tumor cell mass increases the intracranial pressure. This can lead to headaches, vomiting and a steady decline in vision.
Behavioral patterns and personality traits undergo a change, hinting towards such tumors.
Early symptoms may also include seizures. The location of the meningioma determines the extent of additional symptoms.
Frontal Lobe
Tumors located in this lobe lead to subtle variations in personality and mood swings. One-sided paralysis (hemiparesis) is also a possibility.
If the tumor affects the left side of the brain, the patient may experience difficulties with speech, such as slurring or unclear words.

If the temporal lobe is affected, problems of memory loss and coordination may occur.
Changes in one's ability to write, paralysis of one side of the body and seizures are the presenting features of tumors situated in the parietal lobe.
Weakness in the extremities (arms, legs) and loss of hearing ability can be a sign as well. A conclusive diagnosis can be made only after an MRI scan of the brain is performed.
Treatment
The preferred treatment for such meningiomas, especially large ones that grow at a rapid rate and those producing symptoms, is surgery.
The aim of neurosurgery is to excise as much of the mass of aberrant cells as possible. In cases of meningiomas, excision is not always easy due to its size and its risky location (in proximity to vital brain structures).
There is also a possibility that tumors can resurface even after a surgical operation.
In situations in which it is not possible to remove the entire meningioma through neurosurgery, radiation therapy can curb the chances of re-growth.
Complications
There are complications associated with surgery that include the following: the destruction of healthy brain tissue, bleeding, and infection. Other serious complications include:
Temporary Cerebral Edema
There may be a build-up of cerebrospinal fluid in the brain, which is quite common, especially in cases of meningiomas. Patients must take medications both before and after the surgery to prevent such complications.
Seizures
Even for those patients who have never experienced seizures before, brain surgery patients may experience a few attacks after the operation. Anti-epileptic drugs are recommended after the surgery and the dose is tapered gradually until such attacks cease.
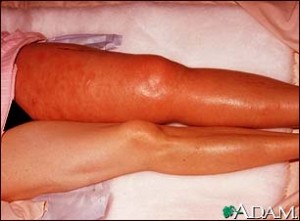
After the partial removal of a meningioma, there is a risk of deep vein thrombosis (blood clots) along with embolisms in the lungs. Blood clots can form in the veins of legs, thighs or lungs.
After the surgery, the patient is given sufficient time to heal. In cases in which the tumor is deep in the brain or close to important blood vessels, radiation therapy is strongly recommended.
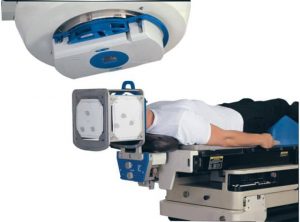
X-rays that are high in energy are aimed at the affected areas. The altered tumor cells exposed to the strong radiation dose will perish. Care is taken to reduce exposure to healthy tissues.
Multiple small doses are administered in fractionated radiotherapy. This treatment continues for at least five days a week for six weeks.
Stereotactic radiosurgery is not a typical treatment. In this treatment, a narrow beam of rays is directed at the targeted area from separate angles.
This ensures delivery of a substantially high radiation dose for faster and more effective results.
Post-surgery, the side effects of radiation therapy are unavoidable. However, they are not life-threatening and can be treated with medication.
After the third week of radiation treatment, loss of hair begins. This change is either temporary or permanent.
Less common after-effects include nausea and headaches. In rare cases, stereotactic surgery causes fatigue and a few episodes of mild headaches.
Driving instructions
In some cases, patients may be advised not to drive a vehicle for a period of time. If you have already experienced a seizure, you will not be allowed to drive for at least one year after the last seizure incident.
Even in benign cases in which there have been no seizures, patients are prohibited from driving for approximately six months after the operation.
Driving large automobiles or those carrying passengers is only possible five years after brain surgery.